Is your Agency ready to embrace the HHVBP Model?
 Introduction
Introduction
Value-based care remains the focal point in the Home Health Care industry. The nationwide rollout of the Home Health Value-Based Purchasing (HHVBP) Model started in 2022 and is now in all 50 states of the USA. HHVBP is a major step forward in value-based care for home health agencies, with this home health trend shifting reimbursement away from volume to the quality of care delivered. CMS has designated 2022 a pre-implementation year, providing training and resources to agencies to help prepare them for success without the risk of losing on payments. 2023 will be the first performance year, and payment adjustments will begin in 2025.
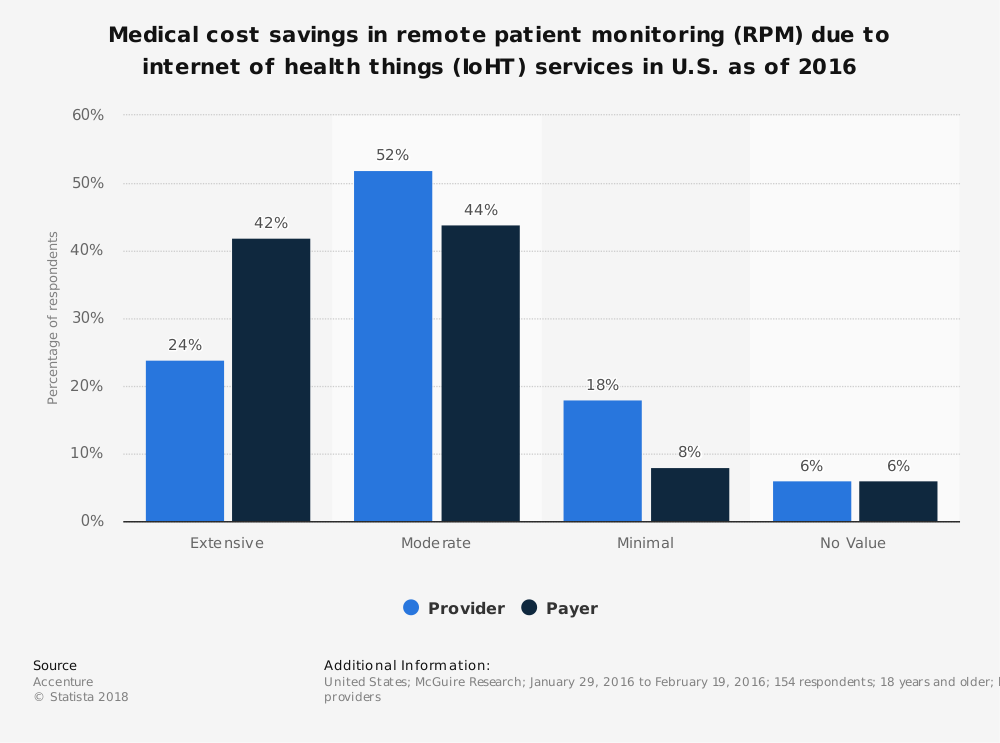
In 2016, the HHVBP pilot model rolled out in nine US states. It was designed to reward agencies with improved quality scores and reduce payments compared to those with lower performance scores. The success of the pilot model has resulted in an average 4.6% improvement in home health agencies’ quality scores and average annual savings of $141 million to Medicare. Agencies following this home health trend also witnessed a reduction in the total cost of care, a significant reduction in unplanned hospitalizations, and patient experience improvement.
HHVBP Model Details
Under the HHVBP Model, HHAs receive adjustments to their Medicare fee-for-service payments based on their:
- Performance against a set of quality measures in relation to their peers’ performance.
- Performance on the quality measures in a specified year (performance year) which impacts payment adjustments in a later year (payment year).
- Data from Outcome and Assessment Information Set (OASIS),
- Surveys from Home Health Consumer Assessment of Healthcare Providers and Systems (HHCAHPS) and claims-based measures are used to calculate HHAs’ performance.
A percentage ranging from -5% to 5% in a payment year is applied toward Medicare fee-for-service payments. In this Model, cohorts are determined based on each HHA’s unique beneficiary count in the prior Calendar Year. HHAs are assigned to either a nationwide larger-volume cohort or a nationwide smaller-volume cohort. HHAs of similar size are more likely to receive scores on the same set of measures to set benchmarks and achievement thresholds to determine payment adjustments.
The main goal of the HHVBP Model
- Provide incentives for better quality care with greater efficiency;
- Study new potential quality and efficiency measures for appropriateness in the home health setting;
- Enhance the current public reporting process.
Pre-Implementation and Education
Agencies that will be subject to the HHVBP program for the first time during the performance year 2023 benefit to learn from those who have adopted the HHVBP Pilot model before. In addition to Department of Health and Human Service materials designed to help address home health agency questions, many other industry resources help agencies adapt.
“This is the time to educate the industry on what to expect,” says Salim Bhinderwala, CEO and founder of Michigan-based Home Health Care App Home Health Notify. “This is the right time to ensure the agency’s systems are in place before 2023, when agencies begin to receive reimbursement adjustments for the first time.”
Many agencies are wondering if the change is just one of many fleeting home health trends, or if following it is a necessity. The HHVPB model has been growing consistently for the past decade. It is here to stay. An emphatic “YES” is the answer! Agencies must educate their staff, understand the quality perspective requirements and work towards getting all their work processes in order.
You should dedicate a small team in your agency to acquire and study the educational literature from the CMS. The educational material could be in many forms, including printed booklets, websites, or participation in webinars. The team should educate the entire staff on the growing home health trends like the HHVPB model, and later work towards implementing the systems, ensuring that all the designated tasks occur within the required timeframe.
Improvement in Quality Measures and Reporting
Certain areas where agencies will need to adapt are tracking and improving quality measures.
· Consumer Assessment of Healthcare Providers and Systems (CAHPS)
· Outcome and Assessment Information Set (OASIS) improvement scores.
· Quality Assurance and Performance Improvement (QAPI) programs
· Certification and Survey Provider Enhanced Reports (CASPER)
These scores heavily underline the importance of improving patient experience, as well as the quality of services delivered in home-based care.
“The agencies should stress scoring well on OASIS, which will be the key to reporting outcome improvements,” Salim says. “If you score a patient incorrectly, it will be hard to show any improvement at the end of the treatment.”
OASIS validation, including the competing factors that play into a patient’s outcome, can provide additional insight into potential areas of patient experience improvement. Assessing these factors, which may include anything from the patient’s family situation and home environment to their access to medication, can offer critical context around each patient’s social determinants of health. This is strongly interconnected to their clinical success.
How can your agency prepare for HHVBP?
HHVBP is inevitable. Agency’s reaction toward change in operations will lead to success. Home-based care agencies still continue to navigate the transition from fee-for-service to a system more focused on the outcome. They can utilize this year for preparation, which will help to maximize Medicare reimbursement. A few tips to follow are:
1. Identify your agency’s baseline
Your agency’s current EMR records and OASIS data can be used as a benchmark for your present standing. Obtain your 2019 baseline data, and use this data as a baseline.
2. Create improvement opportunities
You should prepare your agency for this annual competition. Analyze the trend of your outcomes. You should check if you are trending positively or negatively. Identify the problem areas if your results are favorable, and you still need to achieve the national percentile. Understanding your current position will help you steer your agency toward the required goals for 2023 assessments. It will help you build strategies towards improvement in your OASIS score.
3. Identify your strengths and accept referrals wisely.
It is extremely important to ensure and record that the patient receives the right care at the right time and in the right setting under the HHVBP model. When you look at a referral, try to look beyond the initial revenue potential. When considering a referral, evaluate If you can improve the patient and if they are appropriate candidates for your Home Health Agency. Value-based payments will help the agencies to focus more deeply on referrals, adjust performance patterns, and develop programs that will positively impact the care you’re providing.
4. Patient Satisfaction
HHCAHPS survey records the level of customer satisfaction in your agency. Preparing your staff to communicate with the patients to fill out surveys is essential. Customers are the best teachers. Ask them how to improve your services to receive a 10/10 on the feedback form.
5. OASIS proficiency is a must
OASIS measures will be used to calculate 35% of value-based payment scores for large home health agencies and 50% of scores for small ones. Accuracy in OASIS assessments can have a significant impact on your ratings. However, only a few people like doing an OASIS assessment, educating and training staff to understand the potential impact of this survey. This survey can work positively towards quality measures and value-based purchasing results.
6. Business Intelligence
Business intelligence is extremely critical for HHVBP’s success. Smart technologies that can reflect processes and results will prove to be a catalyst for an agency. It can be very helpful for the agency looking for insights into patients’ clinical records and executing daily processes. Dynamic technology is vital in communication with the team and patients. Data stored can be further analyzed to benefit the patient.
Hence, this becomes critical in providing value-based care.
Popular Articles - Lifestyle Conditions

Value-based care remains the focal point in the Home Health Care industry. The nationwide rollout

By the year 2026, Americans will spend a whopping $5.7 trillion on health care. The…

Running a Home Health Agency requires several investments. The company invests money and resources into…





 Running a Home Health Agency requires several investments.
Running a Home Health Agency requires several investments.