The Patient-Driven Groupings Model (PDGM) is the biggest change for home health agencies in over two decades. The shift to the new model requires agencies to examine patient needs, comorbidities, and referral sources to determine if their case-mix optimizes reimbursement. CMS describes PDGM as an alternative case-mix adjustment methodology that will further the shift to a value-based payment system and ultimately reduce the cost of home healthcare delivery. “The redesign of the home health payment system encourages value over volume and removes incentives to provide unnecessary care,” says Seema Verma, SMC administrator and consultant for Medicare & Medicaid Services. “This home health rule focuses on patient needs and not on the volume of care.”
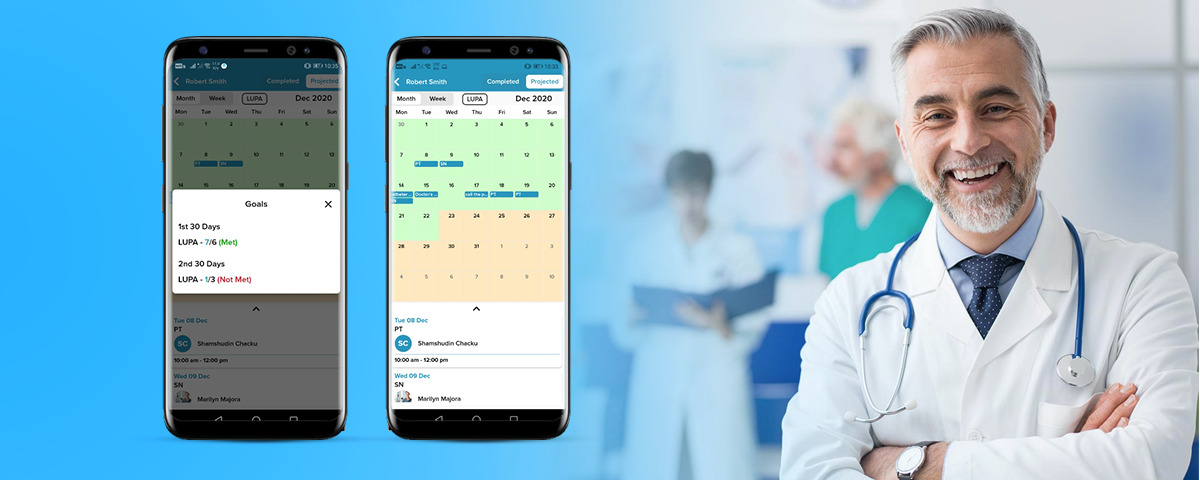
CMS estimates LUPA rates will drop from 8% to 7.1% with PDGM implementation. The policy has dramatically changed home health reimbursement since January 2020. Most crucial area that is important for HHA is cost control while managing care plan of each patient. The change has initiated a shift in CMS’s; hence, care leaders are keen to evolve their organizations into value-driven and client / patient-centred providers.
What it means for HHAs:
The change from 60-day episodes to 30-day periods means that agencies must plan, deliver, document, and bill for care twice as often. The first 24-48 hours from start of care (SOC) will be critical to optimize reimbursement: a HHA clinician must assess the patient’s needs and document a plan of care (POC) as soon as possible.
Today, successfully implementing PDGM requires agency leaders to flex their projecting, planning, and execution muscles. In essence, it’s all about your HHAs ability to manage and execute change effectively. Since the Patient-Driven Groupings Model has taken effect, home health agencies across the country are trying to keep up and maintain compliance. The largest change facing home health agencies in over two decades has many organizations evaluating and updating internal processes. Others are expanding their service lines to serve more clinically complex patients.
PDGM is affecting each agency differently, providers should prepare by adjusting their practices and rebalancing their patient populations. To maximize reimbursements and stay compliant with the model; your organization must have a plan for how to provide effective and efficient care.
Do you have the tools you need to thrive as regulations continue to evolve?
– YES
There are many documented toolkits and programs to train your agency to become PDGM ready. Added pressures from COVID-19 have exacerbated intake challenges. Common issues include missing information in referrals, hard-to-reach referral sources, and gaps in staff knowledge about clinical groupings. You can make your HHAs PDGM ready, but turning them PDGM effective is more vital. It is critical and need of the hour to implement accurate systems to optimise the results of the toolkits and strategies.
The most pertinent option to adopt in these times, when effective change is required, is HOME HEALTH NOTIFY. This e-platform works as a game changer in implementing a much-needed transformation. It is the most organic solution for all HHAs for a revolutionary turn around in efficiency and accountability of staff. This tailor build App will contribute not only in changing the work ethos but also prove an excellent solution for PDGM standards. The Home Health Notify App progressively shifts your agency towards process-oriented systems and efficient staff. Transparent work ethics and real-time results are most favourable to all the levied parties, the patients, the agency and the PDGM policy.